Getting a positive home test brings immense joy to the entire family. Waiting for that first heartbeat, however, brings equal anxiety.
Expectant mothers want absolute clinical certainty. Booking a reliable Pregnancy ultrasound provides exactly that peace of mind.
When your gynaecologist recommends an early Ultrasound scan in Bangalore, the radiologist actively hunts for highly specific developmental markers.
You need a trusted Health screening centre in Bangalore equipped with advanced sonography machines to capture these microscopic changes accurately.
The very first structural sign of a developing embryo inside the womb is called the fetal pole.
It does not look like a baby yet. It appears as a distinct, thick white margin clinging directly to the edge of the yolk sac.
This tiny cellular structure represents the earliest visible stage of new life.
It grows at a rapid, predictable rate of roughly one millimeter every single day.
Doctors measure this specific structure from head to bottom.
Medical professionals call this exact measurement the Crown-Rump Length (CRL).
Finding this specific white margin confirms a viable, healthy pregnancy. It transforms a simple urine test into a confirmed clinical reality for the parents.
When is the Fetal Pole Seen?
Timing is everything in early pregnancy.
Knowing exactly when the fetal pole is seen brings immense relief to expecting parents.
The biological timeline for a developing embryo follows a highly predictable, rapid schedule inside the womb.
A tiny fluid-filled space called the gestational sac appears around four to five weeks.
The circular yolk sac forms shortly after to nourish the new life.
The actual fetal pole finally emerges directly alongside this yolk sac between 5.5 and 6.5 weeks of gestation.
It measures just one to two millimetres at this very first appearance.
Spotting something this microscopic requires the correct diagnostic approach.
The physical placement of the sonography probe completely changes what the radiologist can see.
- Transvaginal Sonography (TVS): The doctor places the ultrasound wand internally. This method provides the highest possible resolution for early detection.
Gynaecologists routinely rely on TVS to clearly identify the fetal pole and a corresponding heartbeat as early as six weeks.
- Transabdominal Ultrasound: The sonographer glides the probe over the mother’s lower belly during a transabdominal ultrasound. This traditional external method usually struggles to detect the tiny fetal pole until at least week seven or eight.
The physical distance and layers of abdominal tissue naturally blur the microscopic details.
Choosing the correct scanning method dictates the clarity of your early results.
Opting for a transvaginal approach during those initial weeks eliminates frustrating guesswork and provides the immediate clinical confirmation families need.
What if the Pole is Missing?
An empty black circle on the sonography monitor causes immediate panic. Expectant mothers often fear a miscarriage right there on the examination table.
Seeing a gestational sac without a visible embryo is incredibly common.
It does not automatically mean the pregnancy failed.
Doctors rely on strict clinical guidelines before declaring a pregnancy non-viable. The most frequent reason for a missing pole is simply incorrect dating.
Many women track their pregnancy using the first day of their Last Menstrual Period (LMP).
This standard calculation assumes a perfect 28-day cycle with ovulation occurring exactly on day 14.
Indian women frequently experience irregular menstrual cycles. Late ovulation pushes the entire biological timeline back by several days or even weeks.
An ultrasound performed at what you believe is six weeks might actually reflect only four weeks of true embryonic development.
At four weeks, the pole remains completely invisible to even the most advanced scanning machines.
The radiologist must consider three specific clinical scenarios when the sac appears empty.
- Delayed Ovulation: Your biological clock started much later than the calendar suggests. The embryo simply needs more time to grow into the visible spectrum.
- Blighted Ovum: Medical professionals call this an anembryonic pregnancy. A fertilized egg successfully implants into the uterine wall and forms a sac, but the actual embryo never develops due to early chromosomal abnormalities.
- Ectopic Pregnancy: The fertilized egg implants outside the uterus, usually in the fallopian tube. The uterine sac appears empty because the embryo is physically growing elsewhere.
Gynaecologists never rush a final diagnosis based on a single early scan. The standard medical protocol requires waiting seven to fourteen days.
A follow-up sonography session allows enough time for the microscopic cells to multiply and finally appear on the monitor.
This waiting period feels agonizing for the family, but it prevents devastating medical misdiagnoses.
Which Week Growth Scan is Done?
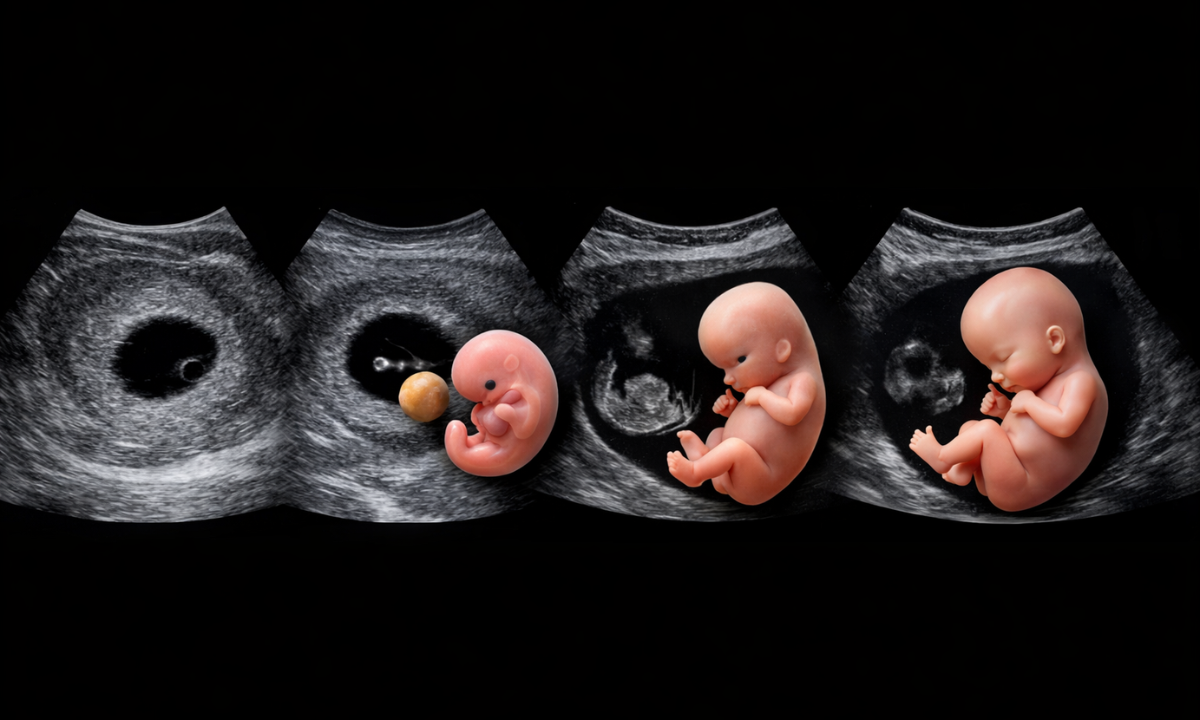
Once the fetal pole and early heartbeat are confirmed, the medical focus shifts completely.
Expectant parents always ask exactly which week the growth scan is done to track their baby’s development safely.
A structured sonography schedule ensures your gynaecologist monitors every critical physiological milestone throughout the three trimesters.
The journey requires specific imaging at highly specific times to catch potential issues early.
The following table outlines the standard diagnostic protocol followed by leading clinics across India.
Table: The Standard Pregnancy Ultrasound Schedule
| Gestational Week Range | Scan Type & Common Name | Clinical Purpose & Focus |
|---|---|---|
| 11 to 13 Weeks | Nuchal Translucency (NT) Scan | Actively screens for major chromosomal conditions like Down syndrome by measuring specific fluid at the back of the fetal neck. |
| 18 to 22 Weeks | Anomaly Scan (Level 2 Ultrasound) | Meticulously examines the physical structure of the developing brain, four-chambered heart, spine, kidneys, and limbs for abnormalities. |
| 28 to 32 Weeks | Third Trimester Pregnancy Growth Scan | Evaluates surrounding amniotic fluid levels, calculates the baby’s estimated weight, and verifies placental position for safe delivery planning. |
Following this predictable clinical roadmap removes immense stress for expecting families.
Regular sonographic monitoring guarantees your doctor can detect and medically manage any late-stage developmental changes immediately.
It transforms abstract pregnancy weeks into visible, reassuring medical data.
Fetal Growth Scan Accuracy and Time
Expectant parents constantly wonder what the sonographer is actually doing during the appointment.
The process involves far more than just looking at a screen.
It requires precise mathematical calculations. Understanding the standard fetal growth scan time helps families prepare mentally for the clinic visit.
A routine sonography session usually lasts between 20 to 45 minutes.
The doctor must carefully measure specific anatomical landmarks to ensure the baby is developing correctly for their exact gestational age.
To determine the overall health and estimated weight of the fetus, radiologists rely on four primary biometric measurements.
Table: Primary Biometric Ultrasound Measurements
| Medical Abbreviation | Full Clinical Term | What The Doctor Measures |
|---|---|---|
| BPD | Biparietal Diameter | The exact diameter of the baby’s head is measured from one side of the skull to the other. |
| HC | Head Circumference | The total distance around the entire perimeter of the developing fetal skull. |
| AC | Abdominal Circumference | The distance around the baby’s belly, which is the most critical metric for calculating fetal weight. |
| FL | Femur Length | The length of the thigh bone is the longest and strongest bone in the human body. |
Variables constantly shift inside the womb. Families must understand that fetal growth scan accuracy is not absolute.
Advanced ultrasound machines calculate estimated fetal weight with a standard error margin of roughly 10 to 15 percent.
A baby predicted to weigh three kilograms might actually be slightly larger or smaller at birth.
Several physical factors directly influence this diagnostic precision inside the clinic.
- Fetal Position: A baby facing the mother’s spine or curled tightly into a ball makes capturing clear cranial boundaries and organ structures incredibly difficult for the sonographer.
- Amniotic Fluid Levels: Fluid acts as a clear acoustic window for high-frequency sound waves. Low amniotic fluid significantly degrades the visual clarity on the monitor.
- Maternal Tissue Density: Increased abdominal tissue physically absorbs the penetrating ultrasound waves, reducing the overall resolution of the internal anatomical images.
These biological limitations explain why gynaecologists never panic over a single slightly off measurement.
Tracking the overall growth curve across multiple appointments provides a far more reliable medical picture than an isolated sonography reading.
Why Choose Koshikaa: Your Diagnostic Partner
Expecting a child requires immense trust in your medical team.
You need a diagnostic partner who understands the deep anxiety behind every single scan. Koshikaa delivers this exact combination of clinical precision and human empathy.
We do not treat expecting mothers like generic file numbers.
- Advanced Sonography Technology: We actively deploy high-resolution transvaginal and abdominal scanning hardware.
This advanced imaging capability allows our specialized radiologists to detect the tiny fetal pole at the earliest possible gestational age.
- Transparent Financials: Hidden medical costs destroy trust.
We clearly outline the exact fetal growth ultrasound price before you even step into the examination room. Expecting families will never face surprise billing for standard biometry tracking.
- Expert Radiologists: Interpreting microscopic embryonic structures requires years of dedicated clinical training.
Our board-certified sonographers strictly adhere to international fetal medicine guidelines to guarantee absolute diagnostic accuracy.
Choosing Koshikaa means securing a flawless medical foundation for your growing baby.
We equip your gynaecologist with the exact biometric data required to manage your pregnancy safely from the first trimester to delivery.
Conclusion
The first few weeks of gestation test the patience of every expecting family.
Waiting to spot that microscopic fetal pole on the sonography monitor feels like an absolute eternity. Biology simply demands time.
The developing embryo will reveal itself only when the gestational age is exactly right.
Do not panic over an initially empty sac. Late ovulation frequently shifts the entire biological calendar backwards by several weeks.
Trust your gynaecologist to map out the correct follow-up scanning protocol. When you are ready to visually confirm your new journey, schedule your diagnostic appointment with Koshikaa.
Our expert clinical team stands ready to guide you through every critical developmental milestone safely.