Our Mammography in Bangalore at Koshikaa helps to get accurate and early breast cancer detection at our advanced scanning centre in Bangalore. We offer screening and diagnostic mammograms, including 3D imaging, for precise results. Book your appointment today.
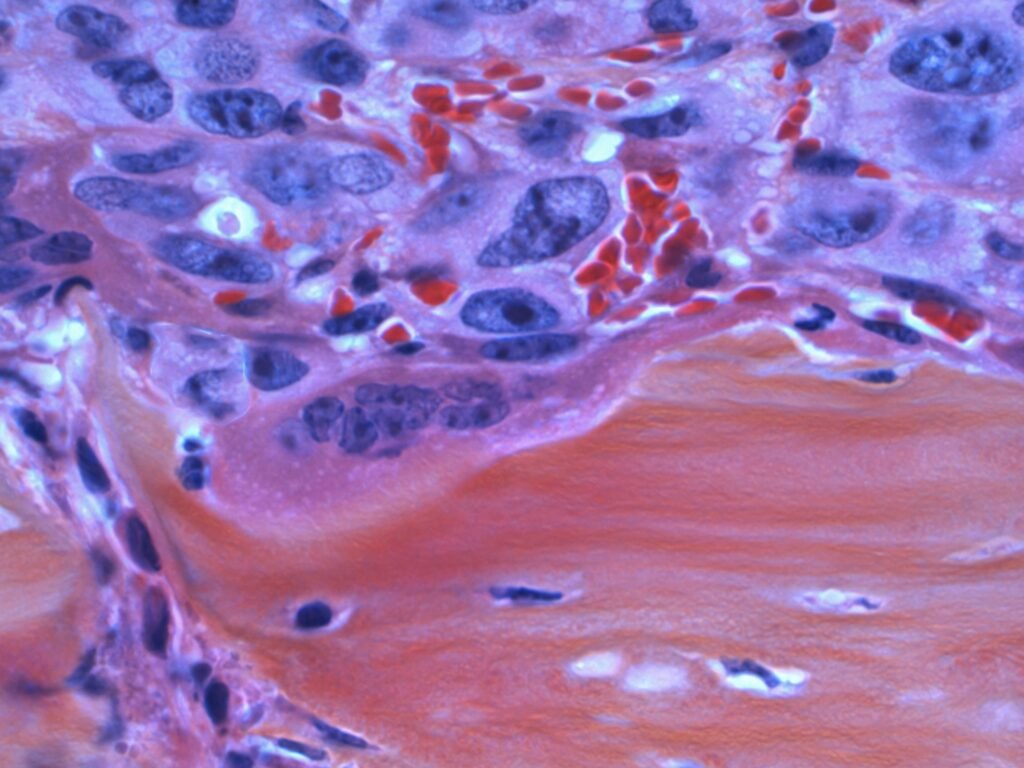
Mammography is a specialized imaging technique used to detect and diagnose breast cancer at an early stage. It utilizes (mammogram is an x ray) low-dose X-rays to capture detailed images of breast tissue, helping radiologists identify abnormalities such as lumps, calcifications, or tumors. Regular mammogram screenings are essential, especially for women over 40 or those with a family history of breast cancer, as early detection significantly improves treatment outcomes. With advancements in technology, digital and 3D mammography provide even more accurate results, reducing false positives and improving diagnostic accuracy.
ur Health Screening Centre in Bangalore offers comprehensive mammography services, including screening and diagnostic mammograms, tailored to individual needs. Our facilities are equipped with advanced imaging technology, ensuring high-resolution scans with minimal discomfort. With an expert team, radiologists provide precise interpretations, guiding patients through the next steps if further evaluation is needed. Whether you require a routine check-up or a detailed breast health assessment, our centre ensures a safe, accurate, and patient-friendly mammography experience. Book your mammogram today for proactive breast health care.
We provide a range of mammography screening designed for early cancer detection and accurate diagnosis of breast conditions. Our screening mammograms are ideal for routine breast cancer checks, recommended for women over 40 or those at risk. For individuals experiencing symptoms like lumps or pain, our diagnostic mammograms offer a more detailed assessment to identify abnormalities with enhanced imaging, reducing false positives and improving accuracy.
A common imaging technique called screening mammography aims to identify breast cancer in asymptomatic women early on, greatly enhancing treatment results and survival rates. Women should get it every year or every two years, depending on their age and risk factors High-resolution imaging, 35% lower radiation than traditional methods, ideal for dense breasts..
Full-field digital mammography (FFDM), another name for digital mammography, takes pictures of the breasts using sophisticated digital detectors. Compared to conventional film mammography, it has several benefits, such as better image quality, better visibility of dense breast tissue, and simpler image storage and retrieval.
Advanced 3D mammography for superior accuracy, detecting 40% more cancers than 2D.
A diagnostic mammogram checks any unusual changes in the breast, such as a new lump, pain, changes in skin texture, nipple thickening, or discharge. It is also used to find out more about unexpected results from a screening mammogram.
Choosing the right scanning centre for your mammogram in Bangalore is crucial for accurate results and a comfortable experience. We offer advanced technology, expert radiologists, and patient-focused care to ensure a seamless screening process.

We use latest equipment, including digital and screening mammography, to ensure accurate and detailed breast imaging for early detection.

Our team of experienced radiologists specialize in breast imaging, providing precise interpretations and expert guidance for your breast health.

We prioritize patient comfort with efficient scanning process, while maintaining the highest safety standards with low-dose radiation technology.

offer flexible scheduling options, allowing you to book your mammogram. Our hassle-free online and phone booking ensures a seamless experience.

streamlined diagnostic process ensures fast turnaround times, so you receive quick and accurate mammogram results for timely treatment planning.

Each patient receives personalized attention, with our experts guiding you through the process, addressing concerns, and recommending further steps.
No special prep needed; avoid deodorants or creams on breasts/underarms. Inform technicians about pregnancy or symptoms (e.g., lumps, pain).
Performed by female technicians in ~10 minutes. Brief compression (5–10 seconds) for clear images; minimal discomfort. Two views per breast, additional for diagnostic cases.
Results delivered digitally or in-person, with expert consultation if needed. Guidance on next steps for abnormal findings.
Minimal radiation, well within safe limits. Advanced equipment reduces exposure by up to 75% compared to traditional systems.
A comfortable and accurate mammography experience can be achieved with proactive preparation. For women without symptoms who want to get screened for breast cancer regularly, the following advice is crucial:
Reviews from Koshikaa Customers
our Mammography is one of the most effective tool for detecting breast cancer at its earliest stages. Early detection increases the chances of successful treatment and recovery.
The test can help identify abnormalities such as lumps, calcifications, or tumors, providing a clear picture. This allows for early intervention and a more precise diagnosis.
Regular mammography screenings are shown to significantly reduce the risk of breast cancer-related deaths, as early-stage cancers are easier to treat and manage effectively.
Advantages of mammography over MRI






Get a safe and accurate mammography with advanced imaging technology and expert radiology care. Our centre provides precise results in a comfortable, private environment to support early detection and proactive breast health.
Visit our centre for professional mammography services focused on precision, and quality care.
Mammography plays a key role in the early detection of breast cancer, which significantly increases treatment success rates. When detected early, breast cancer has a survival rate of over 90%.
Benefits include:
Regular mammograms are one of the most powerful preventive health tools available for women today.
At Koshikaa, we offer advanced options including:
These technologies improve cancer detection by up to 40% when compared to older film mammograms.
The best mammogram depends on your age and symptoms:
| Situation | Best Test |
|---|---|
| Routine screening (40+) | Digital Mammogram |
| Dense breast tissue | 3D Mammogram |
| Lump or pain | Diagnostic Mammogram |
| Additional clarity | Mammogram + Ultrasound |
Our expert radiologists at Koshikaa will guide you to the most suitable option.
Both are important but serve different purposes:
In many cases, both tests are used together for complete evaluation.
The general recommendation is to start routine mammograms at age 40, although women with a family history of breast cancer or other risk factors may need to begin screening earlier. It’s best to consult with your doctor to determine the right time based on individual health needs.
A mammogram typically takes about 15-20 minutes. The actual imaging process is quick, though you may spend some extra time preparing and reviewing your results with the radiologist.
For most women, annual mammograms are recommended starting at age 40. Women with higher risk factors may need more frequent screenings. Consult your healthcare provider for personalized advice on screening intervals based on your health history.
An abnormal result doesn’t necessarily mean you have cancer. It may indicate the need for further tests, such as an ultrasound or biopsy, to determine the cause of the abnormality. Your doctor will guide you through the next steps and discuss any additional screenings or follow-up care needed.
Yes, you can still get a mammogram if you have breast implants. Special techniques are used to ensure the implants do not obstruct the view of the breast tissue, allowing for accurate imaging.
If you’re pregnant or breastfeeding, it’s important to inform your healthcare provider before scheduling a mammogram. Alternative imaging options or adjustments to the procedure may be necessary to ensure both your health and the health of your baby.
If you notice new lumps, pain, or other changes in your breasts, it’s important to contact your doctor immediately. Even if you have had a recent mammogram, any significant changes should be evaluated promptly for proper diagnosis and care.
No, mammography in Bangalore is quite affordable when compared to major cities internationally.
When considering cost, think of:
At Koshikaa, we ensure high-quality scanning at reasonable pricing.
Depending on the type of test selected. 3D mammograms may be slightly higher than 2D digital tests.
At Koshikaa, mammography is priced competitively while maintaining top-tier image quality and diagnosis accuracy.
Estimated range:
(Exact price may vary based on case, appointment time, or combo packages)
Booking is extremely easy:
Our team assists you with smooth scheduling and same-day testing (subject to availability).
Before your test:
Choosing an experienced diagnostic centre with advanced imaging and expert radiologists, like Koshikaa, is also crucial.
Koshikaa stands out as one of Bangalore’s most trusted diagnostic centers for mammography because of:
We are committed to early detection, accuracy, and compassionate care.
Bone X-rays are essential for diagnosing fractures and assessing bone alignment, aiding doctors in developing treatment plans and monitoring healing progress. They provide detailed images of the skeletal system, helping identify abnormalities or injuries that may not be visible through other imaging techniques