When a patient experiences unexplained chest pain, chronic fatigue, or irregular heartbeats, securing a prompt and accurate cardiovascular evaluation is absolutely critical.
Many individuals initially seek an ECG test in Bangalore to measure the electrical activity of their heart muscle. While standard ECG services in Bangalore provide vital data regarding electrical rhythms and conduction speeds, a comprehensive cardiac evaluation frequently requires detailed visual imaging.
For this reason, a premier Health screening centre in Bangalore will often recommend an echocardiogram as the next diagnostic step. Patients frequently ask, What is an echo test, and how does it fundamentally differ from other standard cardiovascular assessments?
While an electrocardiogram strictly measures electrical signals, an echocardiogram utilizes advanced ultrasound technology to create a live, moving image of the physical heart.
This noninvasive diagnostic procedure allows cardiologists to directly observe the mechanical function of the cardiac chambers, the precise movement of the internal valves, and the overall structural integrity of the heart muscle in real time.
To provide absolute clarity for patients preparing for this common diagnostic procedure, this comprehensive guide will detail the clinical realities of the echocardiogram, specifically focusing on the following critical areas:
- Diagnostic Capabilities: We will define the fundamental ultrasound technology utilized to visualize the heart structure.
- Clinical Indications: We will outline the specific physical symptoms and underlying medical conditions that strictly require this visual assessment.
- Procedural Variations: We will categorize the specific types of echocardiograms, detailing how and why cardiologists modify the standard test to gather highly specific anatomical data.
- Interpreting Results: We will explain exactly what structural and mechanical metrics the cardiologist measures during the examination.
Fully understanding the clinical purpose and the exact procedural steps of an echocardiogram, patients can approach their cardiovascular screening with confidence and clarity.
What is an Echo Heart Test?
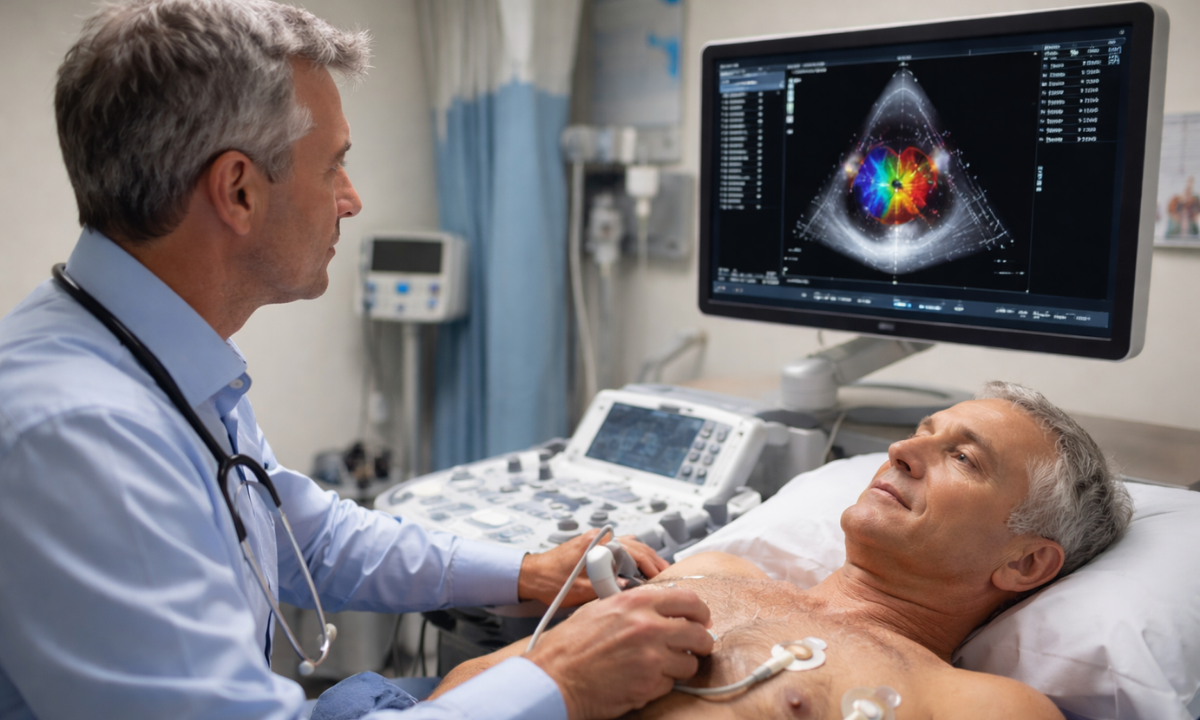
An echocardiogram is a specialized, noninvasive diagnostic imaging modality utilized extensively in modern cardiology.
The procedure relies entirely on the physical properties of high-frequency ultrasonic waves to evaluate the structural integrity and mechanical function of the human heart.
The core technology centers on a handheld medical device known as a transducer. This instrument contains specialized piezoelectric crystals that generate directional sound waves at frequencies far beyond the threshold of human hearing.
During the examination, the sonographer places the transducer directly against the patient’s thoracic wall. The device transmits these concentrated acoustic waves deep into the chest cavity.
As the ultrasonic waves travel through the body, they encounter varying tissue densities within the cardiac structures.
The sound waves physically strike the muscular walls of the heart, the internal valve leaflets, and the circulating blood volume. Upon impact, these waves immediately reflect toward the source. The transducer simultaneously acts as a receiver, capturing these returning acoustic signals.
A connected diagnostic computer instantly processes the exact timing and the precise intensity of every returning echo. The software translates this massive volume of acoustic data into a highly detailed, continuous video display.
This real-time imaging allows the cardiologist to directly observe several critical anatomical and physiological parameters:
- Myocardial Contraction: The exact mechanical pumping action of the left and right ventricles during each cardiac cycle.
- Valvular Function: The precise opening and closing mechanisms of the mitral, tricuspid, aortic, and pulmonary valves.
- Chamber Dimensions: The specific structural size and the internal volume capacity of the atria and the ventricles.
- Pericardial Integrity: The presence of any abnormal fluid accumulation within the protective sac surrounding the heart muscle.
Utilizing sound wave technology rather than ionizing radiation, the echocardiogram provides a completely safe, highly repeatable method for physicians to visualize the internal mechanics of the cardiovascular system.
Why is the Echo Test Done
Cardiologists do not order specialized diagnostic imaging without specific clinical justification. An echocardiogram is strictly indicated when a patient presents with particular physiological symptoms or when a physician detects distinct anatomical abnormalities during a standard physical examination.
Understanding exactly why the echo test is done helps patients recognize the critical nature of their cardiovascular symptoms and the necessity of immediate evaluation.
The decision to proceed with ultrasound imaging is typically driven by a requirement to investigate specific physiological warning signs. The multidisciplinary cardiac team relies on the echocardiogram to either confirm or definitively rule out several dangerous underlying pathologies.
Primary Clinical Indications for Echocardiography
| Patient Symptom or Clinical Finding | Suspected Cardiovascular Pathology | Primary Diagnostic Objective of the Echo |
|---|---|---|
| Unexplained Angina (Chest Pain) | Coronary Artery Disease or a recent Myocardial Infarction (Heart Attack). | To evaluate regional wall motion. Portions of the heart muscle that do not contract normally strongly indicate restricted blood flow and tissue damage. |
| Detection of a Cardiac Murmur | Valvular Stenosis (narrowing) or Valvular Regurgitation (leaking). | To directly visualize the mechanical structure of the valve leaflets and precisely measure the velocity and direction of blood flow utilizing Doppler ultrasound. |
| Chronic Dyspnea (Shortness of Breath) | Congestive Heart Failure or severe fluid overload. | To calculate the Ejection Fraction. This exact metric determines the overall pumping efficiency and volumetric output of the left ventricle. |
| Arrhythmia (Irregular Heartbeat) | Atrial Fibrillation or structural congenital defects. | To assess the specific anatomical dimensions of the cardiac chambers and identify the dangerous presence of potential blood clots (thrombi) pooling within the atria. |
| Severe Peripheral Edema (Swelling) | Right-sided heart failure or Pulmonary Hypertension. | To accurately measure right ventricular function and estimate the internal pressures within the pulmonary artery. |
In addition to diagnosing entirely new cardiovascular conditions, cardiologists frequently utilize this noninvasive imaging modality to actively monitor the biological progression of known diseases over time.
For patients with previously diagnosed valve conditions or those recovering from a major cardiac event, routine echocardiograms provide the exact structural data required.
This continuous clinical surveillance is essential for determining precisely when pharmacological medication dosages require adjustment or when structural surgical interventions become clinically mandatory.
Types of Echo Test
The human cardiovascular system presents unique anatomical challenges for medical imaging. The heart is physically surrounded by dense rib bones and air-filled lungs. Both of these internal structures naturally obstruct high-frequency sound waves.
To overcome these specific anatomical barriers and gather the exact diagnostic data required, cardiologists utilize several distinct types of echo tests.
Each procedural variation is specifically engineered to visualize the cardiac structures from a different physical vantage point or under highly specific physiological conditions.
The diagnostic pathway typically begins with a standard assessment, but the physician will escalate to more advanced modalities if they require higher resolution data or dynamic functional testing.
Clinical Comparison of Echocardiography Modalities
| Echocardiography Modality | Procedural Methodology | Primary Diagnostic Focus | Specific Clinical Triggers |
|---|---|---|---|
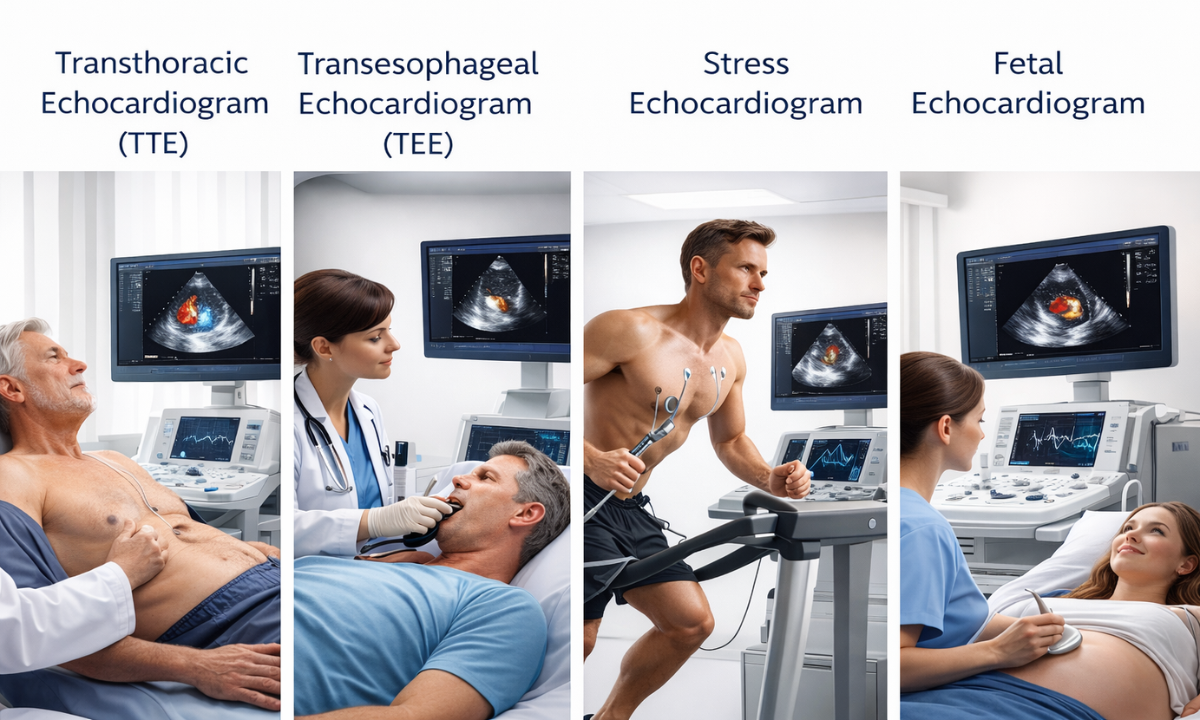
| Transthoracic Echocardiogram (TTE) | Completely noninvasive external chest imaging. The sonographer utilizes a conductive gel and glides a handheld transducer across the thoracic wall. | Provides a comprehensive baseline assessment of chamber dimensions, overall muscle thickness, and standard valve mechanics. | Routine cardiovascular screenings, initial evaluation of newly detected murmurs, or investigating unexplained chest pain. |
| Transesophageal Echocardiogram (TEE) | Minimally invasive internal imaging. The physician utilizes an endoscopic transducer guided directly down the esophagus under local anesthesia and sedation. | Delivers exceptionally high resolution visualization of the posterior cardiac structures by completely bypassing rib and lung interference. | Suspected endocarditis (bacterial valve infections), detection of microscopic atrial blood clots, or precise pre-surgical anatomical mapping. |
| Stress Echocardiogram | Dynamic physiological imaging. Sonographers capture baseline ultrasound images at rest, followed immediately by a second set of images at the absolute peak of monitored cardiovascular exertion. | Facilitates a direct comparison of myocardial wall motion at a resting state versus during maximum physiological demand. | Diagnosing localized restricted blood flow, evaluating severe coronary artery disease, or definitively assessing a patient’s exercise tolerance. |
| Fetal Echocardiogram | Specialized abdominal ultrasound performed exclusively on a pregnant mother, typically during the second trimester. | Evaluates the specific structural development and blood flow patterns of the fetal heart before birth. | Family history of congenital heart disease or abnormal anatomical findings during a routine obstetric ultrasound. |
Categorizing and utilizing these distinct procedural variations, the diagnostic team at Koshikaa ensures that cardiologists possess the precise imaging technology required to evaluate any complex cardiovascular pathology, regardless of anatomical barriers or physical limitations.
The Patient Experience and How the Echo Test is Done
Medical appointments involving cardiovascular diagnostics frequently induce patient anxiety.
However, a standard Transthoracic Echocardiogram is entirely noninvasive, completely painless, and requires zero radiation exposure. Understanding exactly how the echo test is done allows patients to approach their appointment feeling relaxed and fully prepared for the clinical process.
The standard outpatient procedure follows a highly structured, straightforward clinical sequence:
1. Patient Preparation: Upon arriving at the diagnostic center, the patient is escorted to a private examination room and asked to undress from the waist up.
The clinic provides a standard medical gown for comfort and privacy. For a routine resting echocardiogram, there are absolutely no fasting requirements or prior medication restrictions.
2. Clinical Positioning: The patient lies on a comfortable examination table. The sonographer will typically instruct the patient to roll slightly onto their left side.
This specific anatomical posture, clinically known as the left lateral decubitus position, physically shifts the heart closer to the chest wall and widens the spaces between the ribs to allow for optimal sound wave transmission.
3. Concurrent Electrical Monitoring: The sonographer attaches three small adhesive electrode patches to the patient’s chest.
These patches connect to an electrocardiogram monitor, allowing the clinical team to track the precise electrical rhythm of the heart simultaneously alongside the visual ultrasound imaging.
4. Acoustic Gel Application: A specialized, water-based acoustic gel is applied directly to the thoracic wall. This gel serves a critical physical purpose.
As high-frequency sound waves cannot travel efficiently through air, the gel completely eliminates all microscopic air pockets between the patient’s skin and the transducer device, ensuring flawless acoustic transmission.
5. Active Imaging Phase: The sonographer firmly presses the handheld transducer against the gelled skin. They systematically slide and angle the device across multiple specific anatomical landmarks on the chest to capture all required cardiovascular views.
During this phase, the patient may hear loud, rhythmic whooshing sounds from the machine. This audio is simply the Doppler ultrasound function actively measuring the velocity and direction of the internal blood flow.
6. Completion and Recovery: The entire imaging process typically requires thirty to forty-five minutes to complete. Once the sonographer has successfully captured all necessary anatomical data, they wipe away the acoustic gel.
The patient can immediately dress and resume all normal daily activities without any physical restrictions or lingering side effects.
Following this standardized, noninvasive protocol, the clinical team gathers vital cardiovascular data while prioritizing maximum patient comfort.
What Does the Echo Test Show?
Following the completion of the physical imaging phase, a board-certified cardiologist meticulously reviews the recorded ultrasound data.
Patients naturally want to know exactly what the echo test shows and what specific anatomical metrics determine their overall cardiovascular health. The physician analyzes the high-resolution video to evaluate several highly specific physiological parameters.
Key Cardiovascular Metrics Evaluated
1. Ejection Fraction (EF): This is a critical volumetric percentage calculating exactly how much blood the left ventricle actively pumps out into the body with each individual contraction.
A normal ejection fraction typically ranges between 50 and 70 percent. Values falling significantly below this threshold indicate weakened pumping efficiency and potential heart failure.
2. Valvular Hemodynamics: Utilizing the specialized Doppler ultrasound function, the cardiologist measures the exact speed, pressure, and direction of the blood flowing through each of the four cardiac valves.
This precise data immediately identifies severe regurgitation (blood leaking backward) or severe stenosis (stiffening and narrowing of the valve opening).
3. Chamber Hypertrophy: The physician precisely measures the thickness of the ventricular walls.
Chronic high blood pressure frequently forces the heart muscle to thicken abnormally (hypertrophy) to overcome the systemic vascular resistance, which can lead to long-term functional decline.
4. Wall Motion Abnormalities: This specific metric is crucial for patients concerned about a potential heart blockage. It is a common clinical misconception that an echocardiogram visualizes the interior of the coronary arteries.
While the ultrasound cannot see the blocked artery directly, it highly accurately detects the mechanical consequences of that blockage. If a specific segment of the heart muscle receives inadequate blood flow due to an obstructed artery, that targeted tissue will exhibit weakened, delayed, or entirely absent contractions during the scan.
Why Choose Koshikaa for Your Cardiovascular Screening
Accurate interpretation of this complex hemodynamic data requires elite clinical expertise and high-fidelity imaging equipment. Koshikaa provides a superior diagnostic environment specifically engineered to deliver absolute clinical precision:
- Advanced Imaging Technology: We exclusively utilize the latest generation ultrasound machines equipped with advanced Doppler and 3D imaging capabilities, guaranteeing unparalleled anatomical clarity for the reviewing cardiologist.
- Expert Clinical Analysis: Every single echocardiogram performed at our facility is thoroughly evaluated by highly experienced, board-certified cardiologists. This ensures that even the most minute structural abnormalities are accurately identified and documented.
We fully understand the profound anxiety associated with pending cardiac test results. Our streamlined digital infrastructure ensures that comprehensive, highly detailed diagnostic reports are delivered promptly to both the patient and their referring physician to accelerate any necessary medical interventions.
Conclusion
An echocardiogram is a completely safe, highly effective, and entirely noninvasive diagnostic tool that provides invaluable clinical insights into the structural and mechanical health of the human heart. By directly visualizing the active cardiac chambers, valves, and muscle walls, physicians can rapidly detect underlying pathologies and initiate critical medical treatments long before severe cardiovascular complications arise.
If you are experiencing physiological symptoms, require continuous monitoring for a known cardiac condition, or simply need a comprehensive baseline evaluation, contact Koshikaa today. Schedule your expert echocardiogram and secure the precise diagnostic data required to protect your cardiovascular health.