Patients requiring specialized neurological evaluations frequently consult our facility to determine the most clinically appropriate imaging modality. As a premier Health screening centre in Bangalore, Koshikaa strictly prioritizes absolute diagnostic accuracy.
Individuals seeking an X-Ray in Bangalore often possess fundamental misconceptions regarding the specific physical capabilities of standard radiographic technology. When patients arrive at our advanced X-Ray Centre in Bangalore, presenting with neurological symptoms, they frequently present the primary clinical query: Can X-Rays Detect Brain Problems?
Standard radiography is a foundational component of modern medical diagnostics. However, optimizing patient care strictly requires understanding the exact physical mechanics and the absolute clinical limitations of this specific imaging technology.
X-ray beams are a precise form of high-energy electromagnetic radiation engineered to penetrate the human anatomy. The diagnostic efficacy of this fundamental modality depends entirely on the physical density of the specific biological tissue being examined.
To clarify the precise role of standard radiography in neurological assessments, this comprehensive clinical guide will detail three specific diagnostic parameters:
- The Diagnostic Limitation: Explaining the physical interaction between electromagnetic radiation and soft cerebral tissue.
- Skeletal Diagnostics: Defining the strict clinical utility of cranial radiography for identifying structural bone abnormalities following acute physical trauma.
- Advanced Neurological Requirements: Outlining the specific clinical presentations and vascular emergencies that mandate advanced computed tomography or magnetic resonance imaging.
Completely understanding these fundamental physical mechanics, patients can effectively navigate the complex diagnostic pathway and secure the precise radiological evaluation strictly required for their specific clinical presentation.
The Diagnostic Limitation of Soft Tissue Versus Bone
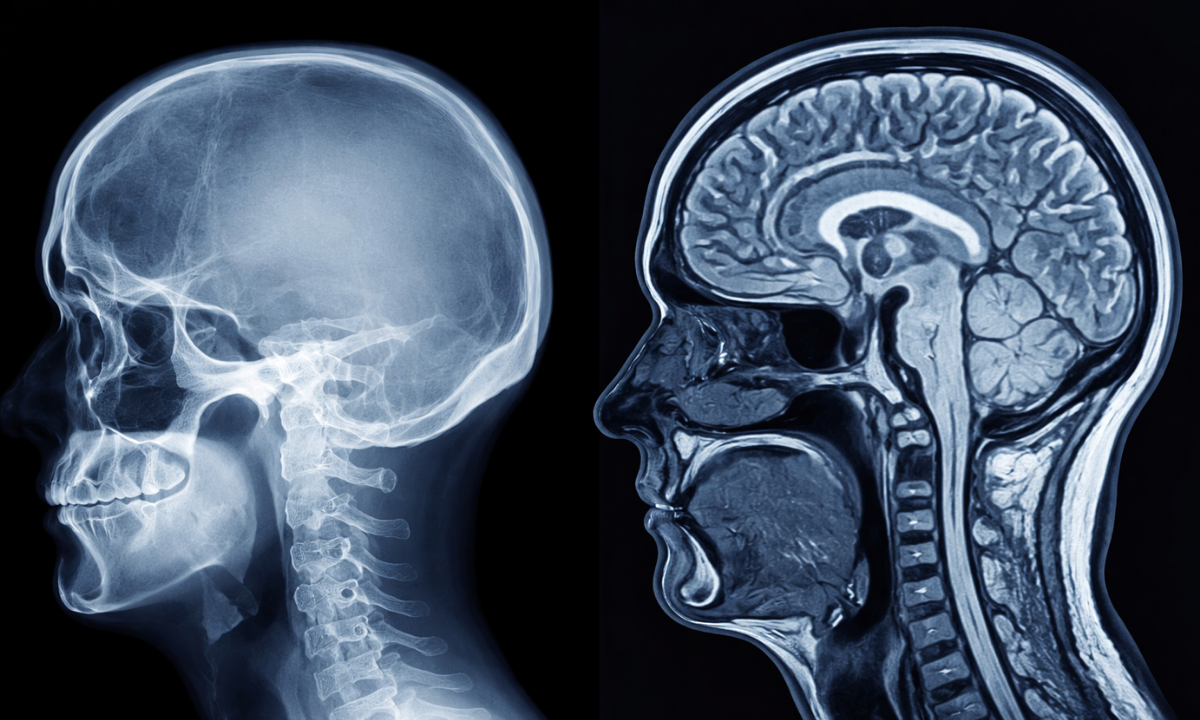
When patients inquire if standard radiographic imaging can detect internal cerebral pathologies, the definitive clinical answer is no.
Standard high-energy electromagnetic radiation cannot capture diagnostic images of the brain itself. The physical mechanics of this imaging modality depend entirely on the specific physical density of the anatomical structures being evaluated.
As the radiation beams pass through the human anatomy, different biological tissues absorb the energy at completely different rates. This differential absorption strictly dictates exactly what appears on the final diagnostic image.
Tissue Density and Radiographic Presentation
| Biological Tissue Classification | Anatomical Example | Radiographic Absorption Rate | Final Image Presentation |
|---|---|---|---|
| High-Density Structural Tissue | Cranial Bone Structure | Maximum Absorption | Solid White |
| Moderate Density Soft Tissue | Cerebral Tissue | Minimal Absorption | Dark Grey or Black |
| Low-Density Elements | Cerebrospinal Fluid | Near Zero Absorption | Pure Black |
As the cerebral tissue and the surrounding internal fluids possess extremely low physical density, the radiation beams pass directly through them without significant physical resistance. Consequently, cranial radiography is clinically blind to the internal soft tissue architecture.
Relying strictly on the physical mechanics detailed in the table above, a standard radiograph is entirely incapable of visualizing the following specific intracranial structures:
- Cerebral Parenchyma: The functional soft tissue of the brain where complex neurological processing occurs.
- Intracranial Vasculature: The highly complex network of internal arteries and veins responsible for cerebral blood flow.
- Ventricular System: The internal anatomical cavities responsible for producing and circulating cerebrospinal fluid.
Identifying pathological alterations within these specific soft tissue structures strictly requires advanced cross-sectional imaging technologies such as computed tomography or magnetic resonance imaging. Standard radiography cannot evaluate the health or physical structure of the brain.
Identifying Skull Fractures
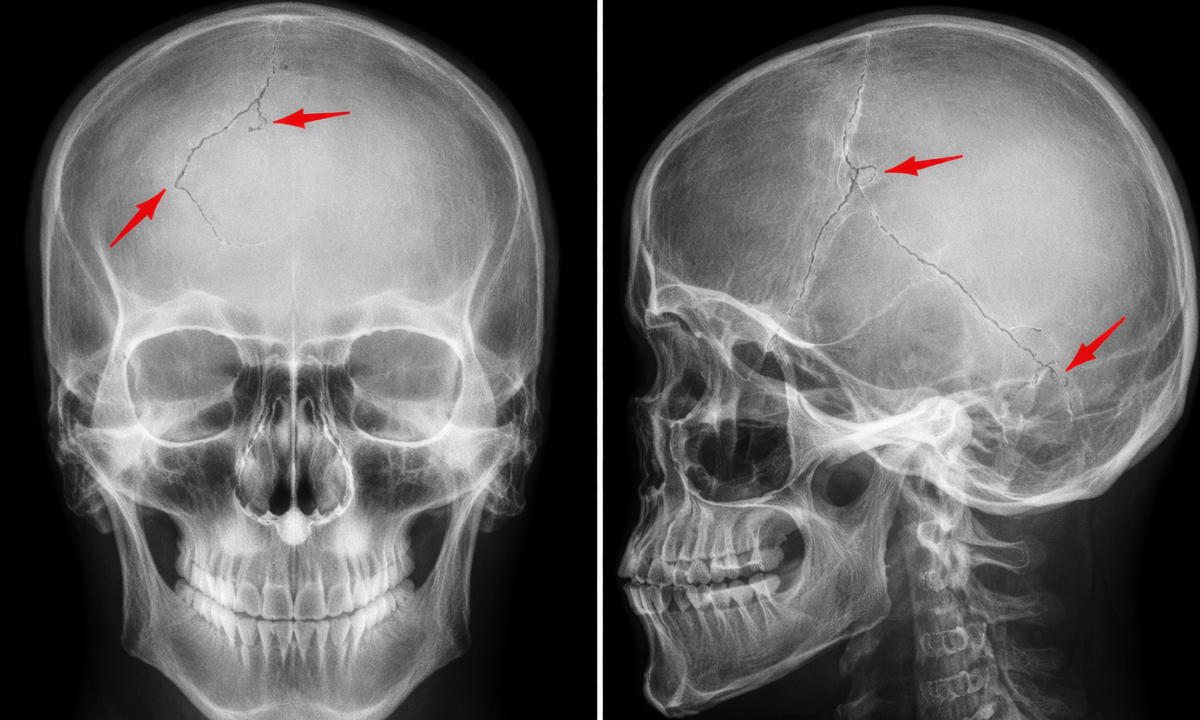
Following acute physical trauma to the head, emergency physicians frequently order a standard cranial radiograph.
While this imaging modality is completely ineffective for evaluating internal cerebral tissue, it remains a highly valuable diagnostic tool for assessing the structural integrity of the surrounding cranial vault.
The primary clinical objective of this specific radiographic evaluation is to identify the physical presence of Skull Fractures.
Because standard electromagnetic radiation is completely absorbed by high-density osseous tissue, standard X-rays provide an exceptionally clear anatomical map of the skeletal structure. Radiologists meticulously analyze these high-contrast images to detect specific structural disruptions within the bone.
Medical professionals categorize these osseous injuries based strictly on their physical presentation on the radiograph.
Clinical Classification of Cranial Fractures
| Fracture Classification | Radiographic Presentation | Clinical Significance |
|---|---|---|
| Linear Fracture | A distinct radiolucent line traversing the cranial bone without any physical displacement of the bone fragments. | Indicates significant blunt force trauma requiring strict neurological observation to monitor for delayed internal bleeding. |
| Depressed Fracture | A focal inward displacement of the cranial bone fragments causes an abnormal physical indentation in the skull contour. | Presents a high risk of direct physical compression against the underlying cerebral tissue, requiring immediate surgical evaluation. |
| Diastatic Fracture | An abnormal structural widening of the natural cranial sutures connecting the individual skull bones. | Frequently observed in pediatric patients following acute physical impacts and indicates significant underlying structural stress. |
Identifying these precise skeletal abnormalities provides critical initial data regarding the exact location and severity of the physical impact.
However, securing this skeletal diagnosis represents only the first phase of a comprehensive trauma evaluation. Even if the radiograph successfully identifies a structural fracture, the medical team must still definitively determine if the underlying cerebral tissue sustained concurrent damage.
Therefore, identifying a fracture on a standard radiograph almost universally mandates immediate advanced cross-sectional neuroimaging to evaluate the internal soft tissue.
Soft Tissue Pathologies of Brain Hemorrhage/Bleeding
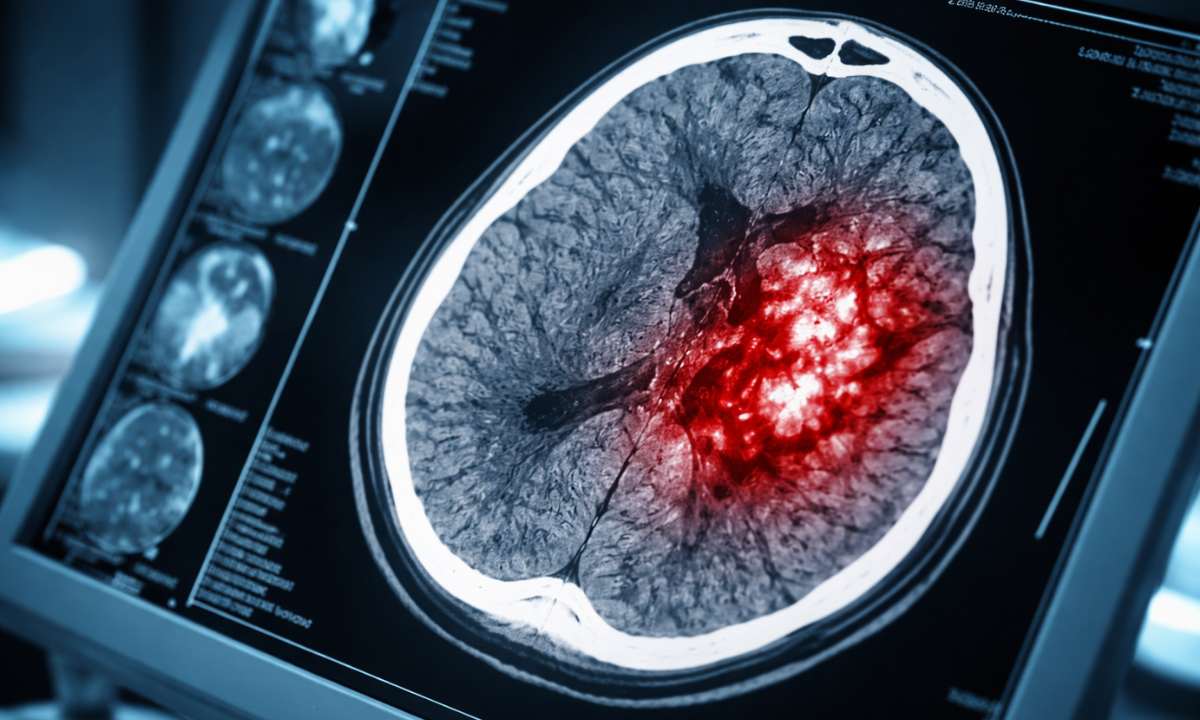
When a patient presents with severe clinical symptoms indicating an acute vascular emergency, such as a Brain Hemorrhage/Bleeding standard cranial radiography is completely ineffective.
A cerebral hemorrhage occurs when an internal blood vessel physically ruptures and actively leaks blood directly into the surrounding functional brain tissue or the anatomical spaces directly beneath the skull.
Because circulating blood and healthy cerebral tissue possess nearly identical physical densities, they absorb electromagnetic radiation at the same rate. Consequently, an active internal hemorrhage and the surrounding brain matter are entirely radiographically indistinguishable. An active bleed remains completely invisible on a standard X-ray.
To secure an accurate diagnosis and prevent catastrophic neurological damage during these critical vascular emergencies, emergency physicians strictly mandate advanced cross-sectional neuroimaging protocols.
The multidisciplinary medical team relies strictly on the following advanced diagnostic modalities to evaluate internal vascular pathologies:
1. Non-Contrast Computed Tomography: This represents the absolute clinical gold standard for evaluating suspected acute cerebral bleeding.
This advanced technology rapidly captures thousands of highly detailed cross-sectional anatomical images. Acute extravasated blood appears significantly denser than normal cerebral tissue on these specific scans. This distinct visual contrast allows the clinical radiologist to immediately pinpoint the exact anatomical location and the precise physical volume of the active hemorrhage.
2. Computed Tomography Angiography: When emergency physicians suspect a ruptured internal arterial aneurysm or a complex arteriovenous malformation, they utilize a specialized intravenous radiopaque contrast agent.
This specific imaging protocol creates a highly detailed structural map of the entire cerebral vasculature, allowing the neurosurgical team to precisely locate the exact anatomical source of the arterial rupture.
3. Magnetic Resonance Imaging: For subacute hemorrhages or highly complex neurological evaluations, physicians utilize advanced magnetic fields and radio frequencies rather than standard ionizing radiation.
This specific diagnostic modality provides unparalleled internal soft tissue contrast. It is strictly required to identify microscopic vascular bleeding or to accurately assess the underlying functional damage to the surrounding cerebral parenchyma.
Completely bypassing standard radiography and directly utilizing these advanced cross-sectional modalities, the medical team ensures rapid and accurate detection of critical intracranial vascular emergencies.
Brain Problems and Symptoms
When evaluating neurological health, medical professionals rely strictly on physical manifestations to determine the necessity of advanced imaging.
Understanding specific brain problems and symptoms empowers patients to seek immediate emergency medical intervention. While standard cranial radiography remains completely ineffective for these soft tissue presentations, identifying common brain problems clinically mandates an immediate computed tomography or magnetic resonance imaging evaluation.
Neurological deficits present in highly specific physical patterns. Physicians categorize these functional manifestations based entirely on their exact anatomical origin within the cerebral cortex.
To secure an accurate diagnosis, the multidisciplinary medical team strictly evaluates the clinical presentation prior to ordering specific radiological scans.
Clinical Correlation of Neurological Deficits
| Specific Clinical Presentation | Potential Neurological Pathology | Strictly Required Imaging Modality |
|---|---|---|
| Acute Unrelenting Cephalalgia | Severe internal intracranial hemorrhage or an actively expanding cerebral neoplasm | Immediate non-contrast computed tomography |
| Sudden Unilateral Motor Weakness | Acute ischemic stroke or a localized severe vascular occlusion | Rapid computed tomography angiography |
| Rapid Cognitive Deterioration | Severe generalized cerebral edema or advanced infectious encephalitis | High-resolution magnetic resonance imaging |
Beyond the specific presentations detailed in the clinical matrix above, emergency physicians also prioritize advanced neuroimaging when patients exhibit any of the following critical functional deficits:
- Severe Visual Disturbances: Sudden unilateral blindness or acute visual field loss indicating severe anatomical pressure on the optic nerve.
- Expressive Aphasia: The sudden physical inability to formulate coherent speech or comprehend spoken language, indicating localized vascular damage to the dominant cerebral hemisphere.
- Motor Seizures: Uncontrolled, aggressive electrical discharges within the cerebral tissue, presenting as severe physical convulsions.
Waiting for these severe physical manifestations to naturally subside is extremely dangerous. Securing an immediate advanced diagnostic scan provides the medical team with the exact anatomical data strictly required to preserve long-term neurological function.
Why Choose Koshikaa? Comprehensive Diagnostic Services at Koshikaa
We recognize that an accurate neurological diagnosis strictly requires utilizing the exact correct imaging modality. Our facility is engineered to provide a complete spectrum of advanced radiological services, ensuring patients receive the precise diagnostic evaluation their specific clinical presentation demands.
By choosing our diagnostic center patients secure direct access to several critical clinical advantages:
- Advanced Multimodality Infrastructure: Our facility houses both state-of-the-art digital radiography systems for immediate skeletal trauma evaluation and highly advanced computed tomography and magnetic resonance imaging scanners for comprehensive internal soft tissue analysis.
- Expert Radiological Interpretation: High-resolution diagnostic data strictly requires specialized clinical analysis. Our dedicated team of clinical radiologists possesses the specific neuroimaging expertise required to accurately identify microscopic vascular bleeding and complex internal cerebral pathologies.
- Integrated Clinical Pathways: We prioritize immediate diagnostic reporting. By streamlining our internal processes, we ensure referring physicians receive precise radiological data rapidly, allowing for the immediate formulation of any necessary medical intervention.
Choosing Koshikaa guarantees access to a highly sophisticated diagnostic environment where clinical precision strictly dictates your comprehensive radiological care.
Conclusion
Navigating a complex neurological evaluation strictly requires adherence to evidence-based diagnostic protocols.
While standard cranial radiography remains a highly effective modality for identifying acute structural skeletal fractures, it is completely incapable of evaluating the internal functional cerebral tissue or detecting severe intracranial vascular emergencies.
Securing an accurate neurological diagnosis strictly depends on matching the specific clinical presentation with the correct advanced cross-sectional imaging technology. If you require a comprehensive diagnostic evaluation or are experiencing severe functional deficits, contact Koshikaa today. Schedule your imaging appointment to secure the precise radiological data strictly required to optimize your long-term neurological health.

