A sudden disruption of cerebral blood flow constitutes an absolute medical emergency requiring immediate diagnostic intervention. Patients seeking a rapid CT scan in Bangalore must secure imaging at a facility specifically engineered for neurological emergencies.
As a highly specialized Health screening centre in Bangalore, Koshikaa understands that every passing minute during a vascular event results in irreversible cellular death. Consequently, administering the correct stroke diagnosis test is not merely a procedural step but the definitive medical action that strictly determines long-term neurological survival.
According to the clinical guidelines established by the American Heart Association and the American Stroke Association, rapid radiological imaging is the absolute foundation of acute vascular neurology.
Emergency physicians cannot administer powerful thrombolytic medications or perform mechanical vascular interventions without first securing precise cross-sectional anatomical data.
To provide absolute clinical clarity regarding these critical emergency protocols, this comprehensive guide will systematically examine the specific radiological pathways utilized during an acute vascular event:
- Clinical Presentation: Detailing the acute physical manifestations of a vascular event and the physiological reality of asymptomatic cerebral damage.
- The Primary Modality: Explaining why non-contrast computed tomography remains the absolute initial standard for emergency stroke evaluations.
- Advanced Vascular Mapping: Differentiating the diagnostic utility of advanced radiological modalities for complex anatomical staging following the initial screening.
Completely understanding these strict evidence-based diagnostic protocols, patients and their families can make highly informed medical decisions during critical neurological emergencies.
Severe Deficits and Silent Infarctions
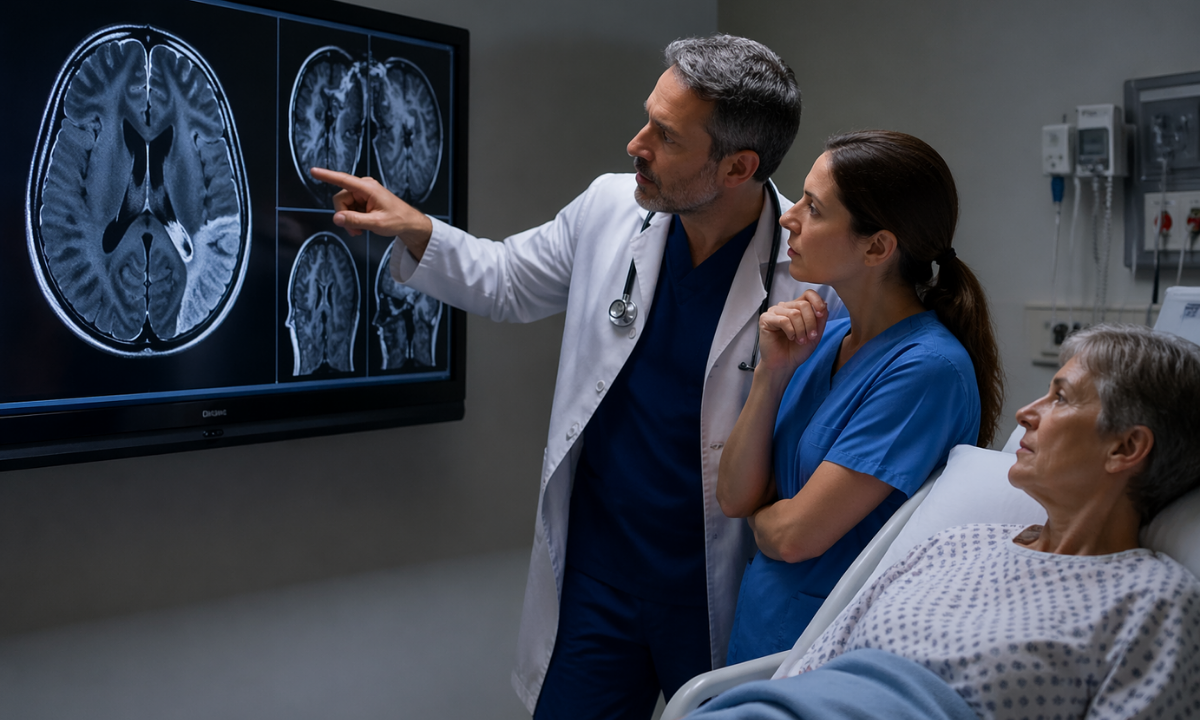
Recognizing a vascular neurological emergency strictly requires observing specific physical manifestations.
When a major cerebral artery experiences a severe structural occlusion, the biological tissue immediately deprived of oxygenated blood rapidly loses its functional capacity. This sudden biological failure produces highly observable physical deficits that clinically mandate immediate diagnostic intervention.
To properly categorize these vascular events, medical professionals divide the clinical presentation into two completely distinct neurological pathways.
Clinical Categorization of Cerebrovascular Damage
| Presentation Category | Pathological Mechanism | Clinical Manifestations | Diagnostic Requirement |
|---|---|---|---|
| Acute Ischemic Event | A sudden severe occlusion within a primary cerebral vessel disrupts major neurological pathways. | Sudden unilateral facial paresis, severe motor weakness in the extremities and acute expressive aphasia. | Immediate emergency cross-sectional neuroimaging. |
| Silent Cerebral Infarction | A highly localized microvascular occlusion occurring deep within non-dominant cerebral structures. | Completely asymptomatic without any immediately observable physical deficits. | Incidental structural discovery during advanced preventative scanning. |
While severe motor deficits strictly dictate immediate emergency action, neurologists also recognize a highly deceptive clinical presentation.
Patients frequently experience a stroke without any symptoms, clinically defined as a silent cerebral infarction. These specific microvascular occlusions permanently destroy small sections of deep cerebral tissue without alerting the patient to the ongoing internal biological damage.
Because these silent infarctions remain completely undetected by the patient, they present a severe long-term clinical risk. The accumulated cellular damage significantly increases the statistical probability of a future catastrophic vascular event and directly contributes to progressive vascular dementia.
Advanced radiological imaging remains the only medical methodology capable of identifying these silent structural lesions before they cause compounding neurological failure.
Standard Stroke Diagnosis Methods

When a patient arrives at an emergency department presenting with severe neurological deficits, medical professionals do not immediately transport them to the radiology department. Securing an accurate vascular evaluation strictly requires a rapid clinical assessment before initiating any advanced imaging. These immediate clinical protocols constitute the foundational stroke diagnosis methods utilized to stabilize the patient and direct the subsequent radiological strategy.
Emergency physicians meticulously execute a standardized clinical pathway. This rapid physical assessment is specifically engineered to rule out other critical biological emergencies and accurately quantify the exact severity of the neurological damage.
Standardized Clinical Assessment Protocols
| Assessment Protocol | Clinical Action | Diagnostic Rationale |
|---|---|---|
| Symptom Onset Verification | Establishing the exact chronological time at which the patient was last observed functioning normally. | Strictly determines patient eligibility for receiving intravenous thrombolytic medications, which possess a highly specific chronological administration window. |
| Capillary Blood Glucose Testing | Rapidly analyzing the systemic blood sugar levels utilizing a precise chemical glucometer. | Severe systemic hypoglycemia directly mimics acute vascular neurological deficits and strictly requires immediate biochemical correction rather than radiological imaging. |
| Neurological Scale Administration | Conducting a standardized physical examination to evaluate specific motor and cognitive functions. | Quantifies the exact severity of the cerebral damage and provides a standardized clinical baseline to measure subsequent biological deterioration or functional recovery. |
| Cardiovascular Stabilization | Securing continuous electrocardiogram monitoring and managing acute systemic hypertension. | Prevents immediate secondary physiological damage and ensures the patient is physically stable enough to safely endure advanced cross-sectional neuroimaging. |
Once the emergency medical team successfully stabilizes the patient and thoroughly documents these precise clinical metrics, the diagnostic priority shifts immediately to structural radiological imaging.
These preliminary physical assessments provide the required clinical context that radiologists strictly utilize to accurately interpret the subsequent neuroimaging data.
CT Scan for Stroke Diagnosis
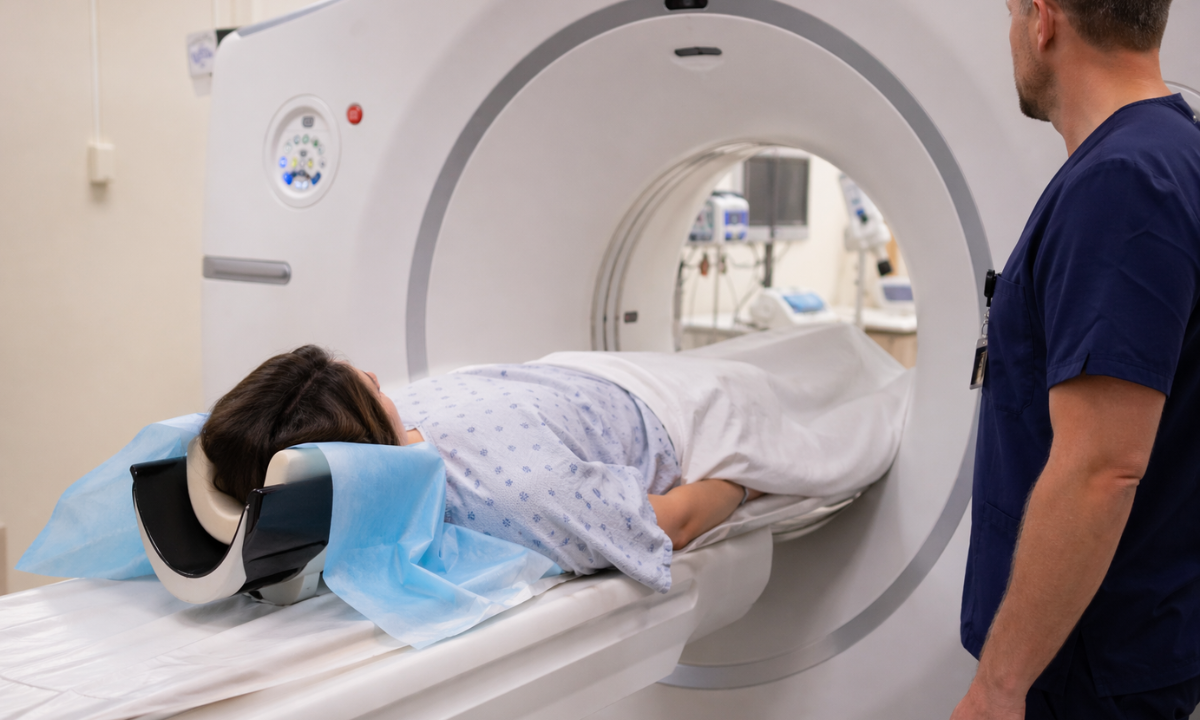
When emergency medical teams evaluate acute neurological deficits, they strictly prioritize a specific cross-sectional imaging protocol.
A non-contrast CT scan for stroke diagnosis represents the absolute universal standard for the initial radiological assessment. This specific imaging modality is not utilized to immediately confirm a microvascular occlusion.
Instead, it serves a much more critical and immediate biological purpose. The primary clinical objective is to definitively rule out the physical presence of an acute intracranial hemorrhage.
Emergency physicians strictly mandate this non-contrast imaging for several highly specific clinical reasons.
- Hemorrhage Identification: Acute extravasated blood appears as a distinct hyperdense region on a non-contrast scan.
Identifying this specific structural anomaly immediately categorizes the event as a hemorrhagic vascular emergency and fundamentally alters the required treatment pathway.
- Pharmacological Safety: Administering intravenous thrombolytic medications to a patient with an active internal bleed is medically catastrophic.
This initial scan guarantees pharmacological safety by physically confirming the complete absence of intracranial bleeding before physicians authorize any chemical clot-dissolving treatments.
- Rapid Image Acquisition: During a severe vascular event, every single minute of cerebral oxygen deprivation results in massive permanent cellular death.
Standard non-contrast scanners acquire complete cranial images in a matter of seconds, ensuring the medical team experiences zero dangerous diagnostic delays.
- Immediate Structural Assessment: Beyond identifying active internal bleeding, this imaging modality rapidly detects other severe physical pathologies.
Radiologists evaluate the images to identify massive cerebral edema or structural midline shifts that strictly mandate immediate neurosurgical decompression.
Utilizing this specific technology as the absolute first-line diagnostic tool, medical professionals safely establish the foundational biological parameters strictly required to proceed with aggressive clinical interventions.
Advanced Vascular Mapping and Identifying the Optimal Stroke Diagnosis Test
After the initial non-contrast scan has definitively ruled out active intracranial bleeding, the medical team must immediately pinpoint the exact anatomical location of the vascular occlusion.
This specific clinical requirement necessitates highly advanced anatomical mapping. Identifying the absolute optimal stroke diagnosis test depends entirely on the specific neurological presentation and the exact elapsed time since the initial symptom onset.
To secure this critical structural data, neurologists strictly select between two advanced cross-sectional imaging modalities. Each technology serves a distinct biological purpose during the acute evaluation phase.
Clinical Comparison of Advanced Vascular Imaging
| Diagnostic Modality | Primary Clinical Function | Targeted Anatomical Structure | Execution Speed |
|---|---|---|---|
| Computed Tomography Angiography | Rapidly maps the entire cerebral vascular network using an intravenous radiopaque contrast agent. | Identifying massive structural blockages within the primary large cerebral arteries. | Extremely rapid, allowing for the immediate authorization of surgical intervention. |
| Magnetic Resonance Imaging | Detects minute changes in internal cellular water diffusion utilizing powerful magnetic fields. | Evaluating deep structural brain tissue and identifying microvascular ischemic damage. | Slower execution requires absolute patient physiological stability. |
Computed tomography angiography remains the definitive standard for evaluating massive structural blockages. This specific test allows neurosurgeons to completely visualize the internal arterial architecture.
Identifying a large vessel occlusion strictly dictates the immediate use of mechanical thrombectomy, where specialized surgeons physically extract the blocking clot directly from the cerebral artery.
Conversely, magnetic resonance imaging provides unparalleled soft tissue contrast. This highly sensitive modality detects microscopic biological cellular damage within minutes of the initial vascular event. Physicians prioritize this specific technology when evaluating highly complex presentations or when they must definitively confirm silent cerebral infarctions that remain completely invisible on standard anatomical scans.
To determine the exact required radiological sequence, the multidisciplinary neurological team strictly evaluates the following critical biological parameters.
- The Chronological Window: The exact measurable time elapsed since the initial symptom onset strictly limits specific pharmacological and surgical interventions.
- Systemic Renal Function: Administering the required intravenous contrast dye strictly requires verified renal chemical stability to prevent secondary acute kidney injury.
- Surgical Tissue Viability: The radiological data must definitively prove that the threatened cerebral tissue remains biologically viable before the medical board authorizes any complex mechanical extractions.
Securing this advanced structural mapping guarantees that the medical team executes the most precise and biologically appropriate neurological intervention.
Why Choose Koshikaa? Specialized Neurological Diagnostics at Koshikaa
At Koshikaa, we recognize that acute vascular emergencies strictly require absolute diagnostic precision and unprecedented clinical speed.
Evaluating severe neurological deficits demands highly advanced radiological infrastructure combined with specialized medical expertise. By choosing our diagnostic center patients secure direct access to several critical medical advantages.
- Rapid Acquisition Infrastructure: Our facility utilizes the latest generation of high-speed computed tomography scanners and advanced magnetic resonance imaging systems. This ensures that every patient receives the highest possible image resolution in the absolute minimum amount of time.
- Specialized Neuroimaging Expertise: High-resolution vascular data strictly requires expert medical analysis. Our dedicated team of clinical radiologists possesses the specific neurovascular expertise required to accurately identify microscopic ischemic damage and complex arterial occlusions.
- Immediate Clinical Reporting: During a vascular emergency, we completely prioritize immediate diagnostic reporting. By streamlining our internal diagnostic pathways, we ensure referring emergency physicians receive precise radiological data instantly. This allows for the immediate authorization of life-saving pharmacological or surgical interventions.
Choosing Koshikaa guarantees access to a highly sophisticated diagnostic environment where clinical speed and absolute precision strictly dictate your emergency neurological care.
Conclusion
Navigating an acute neurological emergency strictly requires an immediate evidence-based medical response. Waiting for severe physical deficits to naturally resolve guarantees massive permanent cellular death. Rapid cross-sectional radiological imaging remains the absolute foundation of early vascular intervention and long-term neurological survival.
If you observe sudden, severe neurological deficits, seek emergency medical intervention immediately. Secure your emergency radiological evaluation at Koshikaa to obtain the precise diagnostic data strictly required to optimize your long term functional recovery.