A comprehensive Full Body checkup in Bangalore often includes a specialized endocrine panel to evaluate the metabolic health of the patient.
As a premier Health screening centre in Bangalore, Koshikaa provides the necessary diagnostic tools to monitor hormonal balance and detect early signs of glandular dysfunction.
When an individual schedules a routine Ultrasound scan in Bangalore or a blood panel, the blood test for tsh t3 t4 serves as the primary screening mechanism for thyroid health. If these biochemical markers indicate an abnormality, the physician will typically order a Thyroid ultrasound in Bangalore to visualize the physical structure of the gland.
The thyroid gland is a small organ located in the anterior neck that produces hormones critical for regulating the body’s energy use, temperature, and heart rate.
As thyroid disorders can manifest with vague symptoms such as fatigue or weight changes, clinical laboratory testing is the only objective method to determine functional status. This blog will provide a detailed examination of the thyroid panel by addressing the following clinical areas:
- The biological significance of the pituitary and thyroid hormones: We will examine how these chemicals interact within a closed feedback loop to maintain systemic homeostasis and metabolic regulation.
- The established reference ranges and clinical interpretations: We will provide the standard laboratory benchmarks to help patients understand the difference between normal and pathological findings in their reports.
- The diagnostic transition from functional to structural testing: We will explain why a blood test is often followed by imaging when a physical anomaly or nodular growth is suspected.
Only by understanding these diagnostic components, patients can take a proactive role in their endocrine health and recognize the importance of regular screening in identifying silent metabolic shifts.
Understanding TSH, T3, and T4
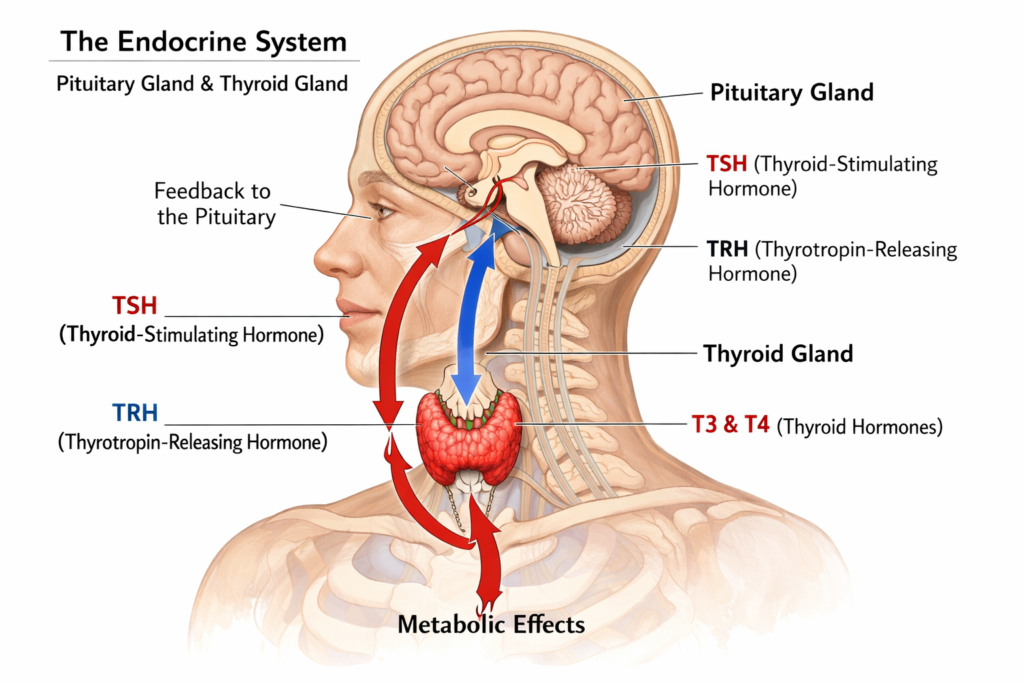
To comprehend the diagnostic utility of a comprehensive thyroid panel, patients must first understand the precise biological feedback loop that regulates systemic metabolism. The human endocrine system utilizes a highly calibrated chemical signaling pathway known as the hypothalamic pituitary thyroid axis.
This biological axis ensures that the body maintains a strict physiological balance of circulating metabolic hormones at all times.
When a physician orders this specific blood test, the clinical laboratory evaluates three distinct hormonal biomarkers. While these chemicals function synergistically to regulate cellular energy, they originate from entirely different anatomical structures within the human body.
The Primary Endocrine Biomarkers
| Biomarker | Anatomical Origin | Primary Physiological Function |
| Thyroid Stimulating Hormone (TSH) | Anterior Pituitary Gland (Brain) | Stimulates the follicular cells of the thyroid tissue to synthesize and release metabolic hormones into the systemic circulation. |
| Thyroxine (T4) | Thyroid Gland (Neck) | Serves as the primary inactive prohormone produced directly by the gland, accounting for approximately eighty percent of total thyroid output. |
| Triiodothyronine (T3) | Thyroid Gland and Peripheral Tissues | Functions as the biologically active hormone that directly interacts with cellular receptors to regulate the basal metabolic rate, heart rate, and body temperature. |
The physiological relationship between these biomarkers operates on a strict negative feedback loop. The concentration of TSH in the bloodstream is inversely proportional to the levels of circulating T3 and T4.
When the pituitary gland detects a decrease in circulating thyroid hormones, it actively increases the secretion of TSH to stimulate greater glandular production.
Conversely, if the thyroid gland autonomously produces an excessive volume of T3 and T4, the pituitary gland immediately suppresses TSH secretion to prevent further hormonal synthesis.
Understanding this inverse biochemical relationship is strictly necessary for interpreting clinical laboratory results. By measuring the pituitary signal alongside the actual glandular output, physicians can precisely identify the exact anatomical source of a metabolic disorder.
Interpreting the Data and Establishing Clinical Baselines

When a clinical laboratory processes a blood sample, the resulting numerical values are compared directly against established physiological reference ranges.
These standardized benchmarks define the normal tsh and t4 values expected within a healthy adult population. By carefully evaluating where a patient’s specific numbers fall within these established tsh t3 t4 ranges, an endocrinologist or primary care physician can objectively determine the functional status of the thyroid gland.
It is critical to note that exact reference ranges fluctuate slightly depending on the specific analytical equipment and chemical assays utilized by the diagnostic laboratory.
However, the global medical community recognizes widely accepted standard parameters for interpreting tsh t3 t4 results. In modern clinical practice, physicians typically rely on “Free” T4 measurements rather than “Total” T4, as the free measurement represents the biologically active hormone that is not bound to carrier proteins in the bloodstream.
Standard Adult Reference Ranges for Thyroid Biomarkers
| Endocrine Biomarker | Standard Adult Reference Range | Clinical Significance of Deviation |
| Thyroid Stimulating Hormone (TSH) | 0.4 to 4.0 mIU/L (milli-international units per liter) | Elevated levels indicate an underactive thyroid (hypothyroidism), while suppressed levels indicate an overactive thyroid (hyperthyroidism). |
| Free Thyroxine (Free T4) | 0.8 to 1.8 ng/dL (nanograms per deciliter) | Abnormal levels confirm the exact severity of the thyroid dysfunction initially identified by the TSH reading. |
| Total Triiodothyronine (Total T3) | 80 to 200 ng/dL (nanograms per deciliter) | Elevated levels are a primary indicator of hyperthyroidism, particularly when T4 remains within normal limits. |
Understanding these clinical baselines provides patients with essential context regarding their metabolic health.
However, a physician must interpret these laboratory results within the specific biological context of the individual patient. Physiological factors such as advanced age, active pregnancy, or the routine use of certain medications like oral contraceptives can significantly alter the normal circulating levels of these hormones.
Therefore, a clinical diagnosis is never formulated solely on isolated laboratory numbers but requires a comprehensive medical evaluation by the referring doctor.
Pathological Patterns and Identifying Hyperthyroidism
When the established biological feedback loop experiences a functional disruption, the resulting laboratory data will display distinct pathological patterns. By analyzing the inverse relationship between the pituitary signal and the peripheral glandular output, physicians can accurately diagnose both overt and early stage metabolic diseases.
The primary objective of the blood test is to determine if the thyroid is overproducing hormones, underproducing hormones, or compensating for an emerging structural defect.
Endocrinologists classify the results into several specific diagnostic categories based on the exact hormonal presentation.
Overt Hyperthyroidism
When the thyroid gland becomes autonomously overactive, it synthesizes and releases an excessive volume of metabolic hormones into the systemic circulation.
The pituitary gland detects this toxic abundance and immediately ceases its production of the stimulating signal to prevent further output. Consequently, the classic laboratory presentation of tsh t3 t4 in hyperthyroidism reveals a severely suppressed or entirely undetectable TSH measurement paired with abnormally elevated concentrations of free T4 and total T3.
This specific biochemical pattern confirms that the origin of the hormone overproduction lies within the thyroid tissue itself.
Primary Hypothyroidism
Conversely, when the thyroid tissue experiences progressive damage due to autoimmune inflammation or structural degradation, the gland loses its capacity to synthesize adequate hormones.
As circulating levels of T3 and T4 drop significantly below normal physiological baselines, the pituitary gland attempts to aggressively stimulate the failing thyroid tissue by secreting massive quantities of TSH.
The resulting diagnostic blood work will demonstrate a highly elevated TSH reading alongside critically low measurements of free T4.
Subclinical Hyperthyroidism
During the earliest phases of glandular overactivity, the pituitary gland is exceptionally sensitive to microscopic increases in peripheral hormone levels.
A patient may present with a suppressed TSH measurement while their actual T3 and T4 levels remain strictly within normal physiological reference ranges. This pattern indicates that the pituitary is actively restricting stimulation to keep the thyroid output from exceeding normal limits.
Subclinical Hypothyroidism
Similarly, early stage glandular failure presents with an elevated TSH measurement paired with strictly normal T3 and T4 levels.
This indicates that the pituitary gland must work significantly harder than normal, pumping out excess stimulation just to force the struggling thyroid to maintain a baseline level of hormone production.
Recognizing these specific biochemical patterns is the critical first step in endocrine disease management.
However, while a blood test perfectly identifies how the gland is functioning, it cannot identify structural causes such as nodules, cysts, or inflammatory swelling.
When the functional data indicates a pathological state, the physician must transition to anatomical imaging to locate the physical source of the dysfunction.
The Role of a Thyroid Ultrasound
While a comprehensive endocrine blood panel successfully identifies the presence of a metabolic disorder, it cannot determine the specific anatomical root cause of the dysfunction.
Hormonal biomarkers provide a strictly functional assessment. If the clinical laboratory results indicate active hyperthyroidism or hypothyroidism, or if the referring physician detects a palpable mass in the anterior neck during a physical examination, the immediate next clinical step is a targeted Thyroid ultrasound.
This non-invasive imaging modality utilizes high frequency sound waves to create a detailed, real time structural map of the endocrine tissue. By transitioning from biochemical testing to anatomical imaging, the interpreting radiologist can visually identify the exact physical pathology driving the abnormal blood work.
The sonogram specifically evaluates the gland for the following structural anomalies:
Nodular Growths
The ultrasound easily differentiates between solid cellular masses and benign, fluid filled cysts.
Identifying the exact composition, size, and borders of a nodule is strictly necessary for determining if a fine needle aspiration biopsy is clinically required to rule out malignancy.
Glandular Enlargement
The sonographer captures precise physical measurements of both the left and right thyroid lobes, as well as the connecting isthmus.
This data definitively confirms the presence and exact dimensions of a structural goiter.
Tissue Inflammation
In autoimmune conditions such as Hashimoto’s thyroiditis or Graves’ disease, the ultrasound reveals a distinct, heterogeneous pattern of tissue degradation.
The radiologist will also utilize a specialized Doppler mode to measure the velocity of the vascular blood flow, which significantly increases during active inflammatory states.
With pairing the functional data from the blood test with the structural data from the sonogram, the endocrinologist gains a complete diagnostic picture.
This combined, evidence based approach allows for the immediate implementation of highly targeted medical therapies, pharmacological adjustments, or necessary surgical interventions.
Why Choose Koshikaa for Your Endocrine Evaluation?
Accurate metabolic diagnostics require precise laboratory analysis paired with advanced imaging capabilities. As a leading diagnostic facility, Koshikaa offers a fully integrated approach to thyroid health.
When patients require a comprehensive endocrine assessment, our clinical infrastructure provides several distinct advantages to ensure a flawless diagnostic experience:
Integrated Diagnostics
We seamlessly bridge the gap between functional laboratory testing and anatomical imaging.
If your blood work reveals a hormonal abnormality, our facility is fully equipped to perform the necessary high resolution sonogram under the same roof, ensuring absolute continuity of care.
Transparent and Accessible Pricing:
We firmly maintain that critical health screenings must remain financially accessible to all patients. Individuals frequently ask about the tsh t3 t4 test price when scheduling their annual medical evaluations.
At Koshikaa, the complete thyroid blood panel is priced highly competitively at five hundred Indian Rupees. Furthermore, this essential biomarker panel is standardly included within our broader preventive health packages.
Rapid Result Delivery:
We utilize highly advanced automated chemical analyzers to process blood samples swiftly and securely. Patients receive their fully verified, highly accurate digital laboratory reports within twenty four hours. This rapid turnaround allows referring endocrinologists to initiate necessary medical therapies without dangerous administrative delays.
Our clinical laboratory strictly adheres to the highest national calibration standards. This rigorous oversight guarantees that every single measurement of your pituitary and glandular hormones is completely objective and clinically reliable.
Conclusion
Maintaining optimal physiological health requires a strictly proactive approach to endocrine monitoring. Because the thyroid gland serves as the primary regulator for fundamental metabolic processes, even minor microscopic fluctuations in hormone production can significantly impact a patient’s daily energy levels, cardiovascular function, and overall systemic homeostasis.
A routine blood test for these critical biochemical markers provides the exact functional data required to detect early stage hyperthyroidism, hypothyroidism, or emerging autoimmune diseases long before severe clinical symptoms physically manifest.
By establishing an accurate clinical baseline of your metabolic function, you directly empower your medical team to make highly targeted, evidence based decisions regarding your long term physiological health. Whether your physician recommends a routine functional laboratory panel or an advanced structural sonogram, Koshikaa is fully prepared to deliver the highest standard of diagnostic precision available.
Protect your metabolic health with accurate, timely clinical data. Contact Koshikaa today at +91 7996666106 or visit our primary diagnostic center in Bangalore to officially schedule your comprehensive endocrine screening.

